Magnesium Chelate or Citrate: What Hematologists Recommend
This article systematically compares the biochemical properties and bioavailability differences between chelated magnesium and magnesium citrate, as well as their therapeutic effects in various health conditions including cardiovascular disease, diabetes, gastrointestinal disorders, and kidney disease. Supported by a detailed comparison table and professional medical advice, it provides evidence-based guidance for making informed choices. It also clarifies the target populations, contraindications, and potential drug interactions of different magnesium preparations, emphasizing the importance of personalized selection based on individual health status and medical consultation to avoid misuse and achieve precise supplementation. Specialized recommendations are provided for pregnant individuals, patients with renal insufficiency, and those taking multiple medications.
Comparative Analysis of Chelated Magnesium and Magnesium Citrate
Chelated magnesium and magnesium citrate are currently among the most popular choices for supplementing this essential mineral, drawing attention from both professionals and consumers. Each form possesses unique properties that determine its efficacy across different physiological conditions. Understanding the fundamental differences between chelated magnesium and magnesium citrate supports informed decision-making to best meet individual health needs.
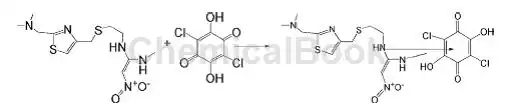
Biochemical Properties of Magnesium Preparations
Chelated magnesium is a compound formed by binding magnesium to amino acids, with a structure resembling a crab’s claw. The magnesium ion sits at the center, surrounded by amino acids that protect it from degradation in the digestive tract.
This structure results in an absorption rate of up to 90%—five times higher than inorganic magnesium forms. Chelated magnesium requires no additional biochemical conversion in the body, eliminating the need for transport molecule synthesis. This makes it particularly suitable for individuals with impaired digestive function or sensitive gastrointestinal tracts.
Magnesium citrate is the magnesium salt of citric acid.
It has a bioavailability of approximately 30–40%, significantly higher than magnesium oxide or magnesium carbonate. In the acidic environment of the stomach, magnesium citrate dissociates into magnesium ions and citrate ions, which are then absorbed in the small intestine. The citrate form exhibits osmotic activity, drawing water into the intestinal lumen.
Efficacy in Cardiovascular Disease
In hypertension management, chelated magnesium demonstrates advantages due to its stable and long-lasting effects. A 2010 study showed that chelated magnesium improved blood pressure readings by 15–20%, compared to 10–15% with magnesium citrate.
Magnesium regulates vascular tone and cardiac electrical conduction. Chelated magnesium forms—especially magnesium glycinate and magnesium taurinate—exert notable cardioprotective effects. Magnesium taurinate is specifically recommended for myocardial support in patients with heart failure and angina pectoris.
Magnesium citrate is effective in preventing arrhythmias and reducing arterial wall stiffness.
Research indicates that magnesium citrate helps restore arterial elasticity and lower atherosclerosis risk. It also provides core cardioprotective benefits: stabilizing heart rhythm, normalizing blood pressure, and exerting anticonvulsant effects.
Use in Diabetes
Magnesium deficiency affects 25–38% of patients with type 2 diabetes. Low magnesium levels are linked to insulin resistance and impaired insulin secretion.
Chelated magnesium shows particular efficacy in diabetes management by improving tissue insulin sensitivity. Magnesium glycinate, gentle on the gastrointestinal tract, is suitable for long-term use in diabetic patients who often experience digestive issues. Studies show chelated magnesium increases blood mineral levels by 8.7% while reducing inflammatory markers.
Magnesium citrate also performs well in glycemic control.
Clinical trials demonstrate that supplementation with 1000 mg magnesium oxide or 300 mg magnesium chloride improves glycemic control in poorly controlled diabetic patients. With high bioavailability, magnesium citrate effectively corrects magnesium deficiency and aids blood sugar regulation. A key benefit is its ability to improve lipid profiles by lowering triglyceride and cholesterol levels.
Magnesium participates in over 300 enzymatic reactions, including glucose metabolism. Diabetic patients experience increased urinary magnesium loss, worsening deficiency and creating a vicious cycle. Both chelated magnesium and magnesium citrate can break this cycle, but selection depends on individual tolerance and accompanying symptoms.
Effects on Gastrointestinal Function
Magnesium citrate exerts a pronounced laxative effect due to its osmotic activity.
It draws water into the intestinal lumen, softening stool and stimulating peristalsis. Effects typically occur 30 minutes to 3 hours after administration, making it the first choice for chronic constipation and intestinal motility disorders.
Chelated magnesium rarely causes gastrointestinal side effects. It does not alter gastric acid concentration or irritate mucous membranes. Magnesium glycinate is especially suitable for those with sensitive stomachs, irritable bowel syndrome, or gastroesophageal reflux disease.
When choosing magnesium for gastrointestinal conditions, the primary issue should guide selection.
If constipation is the main concern, magnesium citrate is optimal. For high acidity, heartburn, or diarrhea-prone individuals, chelated magnesium is preferable. Magnesium malate is also well-absorbed and rarely causes gastrointestinal distress, though it may have mild laxative effects.
Application in Kidney Disease
The kidneys play a central role in magnesium homeostasis by excreting excess magnesium in urine. This function is impaired in chronic kidney disease (CKD).
In early CKD stages (1–3), the body compensates by increasing fractional magnesium excretion via glomerular filtration. However, as the disease progresses (creatinine clearance <30 mL/min), compensatory mechanisms fail and hypermagnesemia develops. Excess magnesium is common when creatinine clearance falls below 10 mL/min.
Magnesium citrate is contraindicated in severe renal failure.
It should be avoided in patients with significant renal impairment to prevent dangerous magnesium accumulation. Hypermagnesemia can lead to severe complications: muscle weakness, cardiac arrhythmias, and respiratory depression.
Chelated magnesium also requires caution in kidney disease, especially advanced CKD. Stage 4–5 CKD patients should not take magnesium supplements without blood magnesium monitoring and nephrologist consultation. Even highly absorbable chelated magnesium can cause toxic mineral buildup with reduced renal function.
Paradoxically, research suggests magnesium may benefit early CKD.
Adequate magnesium levels may slow disease progression, reduce vascular calcification, and lower cardiovascular risk. However, magnesium use in CKD must occur under strict medical supervision with regular laboratory monitoring.
Effects on Neurological and Psychiatric Disorders
Chelated magnesium—particularly magnesium glycinate—exerts significant neuroprotective properties through synergistic effects of magnesium and glycine.
Glycine is an inhibitory neurotransmitter involved in serotonin and GABA production, which regulate mood and sleep cycles. This combination makes magnesium glycinate highly effective for anxiety disorders, insomnia, and chronic stress. Patients report improved sleep quality by the third day of taking two tablets before bedtime.
Magnesium L-threonate is the only form that crosses the blood-brain barrier and directly increases brain magnesium concentrations. Animal studies show potential for improving cognitive function and memory, suggesting benefits for age-related cognitive decline and neurodegenerative diseases.
Magnesium citrate also has sedative effects, though less pronounced than magnesium glycinate.
It is effective against migraines—studies indicate a 600 mg daily dose of magnesium citrate can prevent or reduce migraine severity. The mechanism involves magnesium’s influence on cerebral vascular tone and neuronal excitability.
In diabetic peripheral neuropathy, a common comorbidity, intracellular magnesium levels are reduced. Research shows intracellular magnesium content is 1.2±0.5 μg/mg protein in diabetic neuropathy patients, compared to 1.5±0.6 μg/mg in non-neuropathic diabetics. Long-term chelated magnesium supplementation helps restore intracellular stores and may alleviate symptoms.
Use in Musculoskeletal Disorders
Magnesium plays a critical role in muscle contraction and relaxation.
Deficiency increases muscle fiber excitability, leading to twitching and cramps. Chelated magnesium—especially magnesium malate—shows high efficacy for muscle pain and fibromyalgia. Malate in magnesium malate participates in the Krebs cycle, promoting ATP production, the primary energy source for muscles.
Athletes often use magnesium malate to relieve muscle fatigue after intense exercise. It should be taken during the day, however, as malate stimulates energy metabolism and may disrupt sleep if taken at night.
Magnesium citrate effectively treats nocturnal leg cramps common in the elderly and pregnant individuals.
Its rapid absorption provides relatively fast symptom relief. Dosage must be adjusted individually to account for its laxative effect.
Both forms support bone health. Approximately 60% of total body magnesium is stored in bone, influencing osteoblast and osteoclast activity. Long-term magnesium supplementation improves bone mineral density, especially when combined with vitamin D and calcium.
Applications in Women’s Health
Premenstrual syndrome (PMS) is often accompanied by reduced magnesium levels.
Studies show magnesium citrate supplementation produces mild but statistically significant improvements in PMS symptoms. Magnesium and calcium levels fluctuate across the menstrual cycle, reaching their lowest in the premenstrual phase. Additional magnesium relieves pain, edema, and mood swings.
For prominent psychological PMS symptoms—irritability, anxiety, sleep disturbances—magnesium glycinate is preferable. Its sedative effect stabilizes mood without causing drowsiness.
Magnesium requirements increase during pregnancy.
The mineral is vital for normal fetal development, preeclampsia prevention, and reducing preterm birth risk. Chelated magnesium is preferred due to better tolerance and absence of gastrointestinal side effects that may worsen morning sickness. Any magnesium use during pregnancy requires medical consultation.
In menopause, magnesium helps manage hot flashes, improve sleep, and support bone health. Combining magnesium with vitamin B6 enhances efficacy in managing menopausal symptoms.
Drug Interactions
Magnesium supplements may interact with various medications, altering their effects or increasing side effects.
Tetracycline and quinolone antibiotics form chelate complexes with magnesium, reducing absorption of both substances. A dosing interval of at least 2–4 hours is recommended between magnesium and these antibiotics.
Bisphosphonates for osteoporosis interact poorly with magnesium supplements.
Magnesium may reduce bisphosphonate absorption and therapeutic efficacy, requiring a minimum 2-hour interval.
Diuretics exert variable effects on magnesium levels. Loop and thiazide diuretics increase urinary magnesium loss, raising deficiency risk, while potassium-sparing diuretics may promote magnesium retention. Long-term diuretic therapy often requires magnesium supplementation with blood magnesium monitoring.
Long-term use of proton pump inhibitors (PPIs) may cause hypomagnesemia.
PPIs disrupt active intestinal magnesium absorption by altering transporter expression. Patients on long-term PPI therapy should monitor magnesium levels and supplement if needed. Chelated magnesium is preferable, as its absorption is less dependent on gastric acid concentration.
Practical Selection Advice
Choice between chelated magnesium and magnesium citrate should be based on individual physiology and supplementation goals.
Chelated magnesium is suitable for long-term use in chronic conditions requiring consistent deficiency correction without side effects. It is ideal for those with sensitive GI tracts, anxiety disorders, and sleep disturbances. Magnesium glycinate is a versatile choice for most cases. Magnesium malate is better for muscle pain and chronic fatigue syndrome. Magnesium taurinate is recommended for cardiovascular patients.
Magnesium citrate is effective in acute situations requiring rapid magnesium elevation.
It is the preferred choice for constipation-prone individuals, migraine sufferers, and those with PMS. Magnesium citrate is conveniently available in powder form, soluble in water for enhanced absorption and precise dosing.
Dosage depends on therapeutic goals: 200–400 mg of elemental magnesium daily for deficiency prevention, and 600–800 mg under medical supervision for treating deficiency or specific conditions. Note varying elemental magnesium content by salt: magnesium glycinate 10–14%, magnesium citrate 12–16%, magnesium malate ~15%.
Timing of administration is also important.
Sedating chelated forms (magnesium glycinate) are best taken in the evening. Magnesium malate should be taken in the morning or daytime due to its stimulatory effects. Magnesium citrate may be taken at any time, with consideration for its laxative potential.
Safety and Side Effects
Magnesium supplements are considered safe at recommended doses. The adult upper limit for supplemental magnesium is 350 mg daily, though therapeutic doses may be higher under medical supervision.
The most common side effect is diarrhea, particularly associated with magnesium citrate, magnesium carbonate, and magnesium oxide.
Chelated magnesium causes fewer gastrointestinal disturbances. If diarrhea occurs, reduce dosage or switch forms.
Overdose symptoms include nausea, vomiting, hypotension, muscle weakness, and depressed reflexes. Severe hypermagnesemia can lead to respiratory muscle paralysis and cardiac arrest. Overdose risk is minimal in those with normal renal function, as excess magnesium is rapidly excreted in urine.
Absolute Contraindications to Magnesium Intake
Magnesium administration in any form is strictly prohibited in certain conditions.
Severe renal failure is the primary contraindication. With creatinine clearance <30 mL/min, magnesium cannot be adequately excreted and accumulates to toxic levels. Hypermagnesemia develops rapidly in end-stage CKD.
Myasthenia gravis—an autoimmune disorder characterized by pathological muscle fatigue.
Magnesium may worsen muscle weakness by blocking neuromuscular transmission. Even therapeutic doses can trigger acute deterioration, including respiratory failure, in myasthenia gravis patients.
Second- to third-degree atrioventricular block is an absolute contraindication. Magnesium slows atrioventricular conduction, potentially leading to complete heart block and cardiac arrest. First-degree block requires extreme caution with ECG monitoring.
Marked bradycardia (heart rate <50 bpm) precludes magnesium use.
The mineral exerts negative chronotropic effects, further slowing heart rate—particularly dangerous in sinoatrial node dysfunction and with beta-blocker use.
Hypermagnesemia of any cause is a clear contraindication to additional supplementation. This rare condition typically occurs in renal failure or massive magnesium overdose, requiring immediate discontinuation of all magnesium-containing preparations and administration of the antidote: calcium gluconate.
Relative Contraindications and Precautions
Magnesium requires caution in moderate renal insufficiency (creatinine clearance 30–60 mL/min).
Regular blood magnesium monitoring, dosage adjustment, and selection of forms with minimal systemic absorption are necessary. Low-dose chelated magnesium is preferred.
Heart failure with significant hemodynamic impairment requires cautious magnesium prescribing. Renal hypoperfusion in decompensated circulation may cause magnesium retention; additionally, magnesium’s vasodilatory effects can worsen hypotension.
Intestinal dysmotility and chronic diarrhea restrict magnesium citrate use.
Its osmotic effects may exacerbate diarrhea, leading to dehydration and electrolyte imbalances. Chelated magnesium without laxative effects is preferred in these cases.
Children under 12 are contraindicated for many magnesium preparations per labeling, due to insufficient clinical safety data. Pediatric magnesium use, if necessary, should only be prescribed by a physician with weight-based dosing.
Special caution is needed when combining magnesium forms. Some individuals take magnesium glycinate for sleep and magnesium citrate for bowel regularity. Total elemental magnesium dosage must be monitored to avoid overdose. Starting with minimal doses and gradually increasing while monitoring physiological response is safer.
Comparison Table
表格
| Feature | Chelated Magnesium | Magnesium Citrate |
|---|---|---|
| Chemical Structure | Magnesium bound to amino acids (glycine, lysine, arginine) | Magnesium salt of citric acid |
| Bioavailability | 90% – highest among all forms | 30–40% – high among salt forms |
| Elemental Magnesium Content | 10–14% (magnesium glycinate) | 12–16% |
| Absorption Speed | Gradual, stable | Rapid (30 minutes–3 hours) |
| Gastrointestinal Impact | Non-irritating to mucosa; does not alter acidity | Osmotic effect; may cause diarrhea |
| Laxative Effect | None or minimal | Pronounced; used for constipation |
| Tolerance in Sensitive Stomachs | Excellent | May cause discomfort |
| Effects on Stress & Anxiety | High (especially magnesium glycinate) | Moderate |
| Impact on Sleep | Significantly improves sleep quality | Moderately improves |
| Use in Diabetes | Suitable for long-term use | Effective; improves lipid profile |
| Cardiovascular Efficacy | Lowers BP by 15–20%; cardioprotective | Lowers BP by 10–15%; prevents arrhythmias |
| Migraine Use | Moderate efficacy | High efficacy (600 mg daily) |
| PMS Use | Effective for psychological symptoms | Clear improvement in physical symptoms |
| Muscle Cramps | Effective (especially magnesium malate) | Rapid relief for nocturnal cramps |
| Administration Time | Evening (glycinate); morning (malate) | Anytime, accounting for laxative effect |
| Dosage Forms | Tablets, capsules; rarely powder | Tablets, capsules, powder, solution |
| Price | 30–50% more expensive | Moderate, affordable |
| Need for In Vivo Conversion | Not required | Requires dissociation into ions |
| Renal Accumulation Risk | Minimal | Moderate |
| Food Interactions | May be taken independently of food | Best taken with or after meals |
| Main Contraindications | Severe CKD, myasthenia gravis, AV block, bradycardia | Same as above + intestinal dysmotility, diarrhea |
| Pregnancy Profile | Preferred due to absence of side effects | May worsen morning sickness via GI effects |
| Pediatric Use | Syrup form available from age 3 (prescription only) | Use with caution due to laxative effect |
| Treatment Duration | Suitable for continuous use | Best used in cycles due to intestinal effects |
| Compatibility with Other Minerals | Combines well | May interfere with calcium and iron absorption |
Frequently Asked Questions
Can magnesium be taken long-term or should it be cycled?
Physician response: Duration of magnesium intake depends on goals and formulation. Typically, 2–3 months of continuous use is needed to achieve body saturation, followed by a 1–2 month break. Residents of urban areas, diabetics, smokers, and alcohol consumers should complete 2–3 courses yearly due to higher magnesium depletion. Chelated magnesium is suitable for extended use due to minimal GI side effects, while magnesium citrate is best used in cycles because of its laxative properties.
I developed diarrhea the day after starting magnesium citrate. My doctor says to continue. Should I switch to chelated magnesium?
Gastroenterologist response: Significant diarrhea from magnesium citrate is a clear indication to switch formulations. Transitioning to chelated magnesium is appropriate in your case. Magnesium glycinate rarely causes gastrointestinal disturbances and is suitable for those with sensitive digestive systems. Start with a low dose—200 mg daily—and gradually increase to therapeutic levels. If intestinal issues persist, magnesium malate is another well-tolerated option.
I’m taking antibiotics for bronchitis. Can I take chelated magnesium to support my body?
Physician response: Yes, magnesium can and should be taken during antibiotic therapy, as antibiotics exacerbate magnesium depletion. However, strict dosing intervals must be observed. If taking fluoroquinolones (ciprofloxacin, levofloxacin) or tetracyclines, allow at least 3 hours between antibiotics and magnesium. These drugs form insoluble complexes with magnesium, reducing efficacy of both agents. A 2-hour interval is sufficient with other antibiotic classes.
I am 68 years old with early renal insufficiency (creatinine 110). My cardiologist prescribed magnesium for heart health. Which form is safer?
Nephrologist response: Magnesium may be used cautiously in early CKD with creatinine 110 μmol/L. Prioritize low therapeutic doses of chelated magnesium—no more than 200 mg elemental magnesium daily. Monitor blood magnesium levels every two months. Avoid magnesium citrate due to higher systemic absorption. If hypermagnesemia symptoms occur—severe drowsiness, muscle weakness, slow pulse—discontinue use immediately and seek medical care. Note that magnesium may become contraindicated as renal insufficiency progresses.
I experience severe irritability and edema with PMS. A friend recommended magnesium citrate, while online sources suggest magnesium glycinate. Which works better for my symptoms?
Gynecologist response: Magnesium selection for PMS depends on predominant symptoms. For psychological symptoms (irritability, anxiety, tearfulness), magnesium glycinate is optimal. Glycine enhances magnesium’s sedative effects, improving sleep and stabilizing mood. For physical symptoms—edema, breast tenderness, headaches—400 mg daily magnesium citrate, starting 7–10 days before menstruation, is more effective. Combination use is possible: morning magnesium citrate to reduce edema, evening magnesium glycinate to improve mood. Total daily elemental magnesium should not exceed 400–450 mg.
